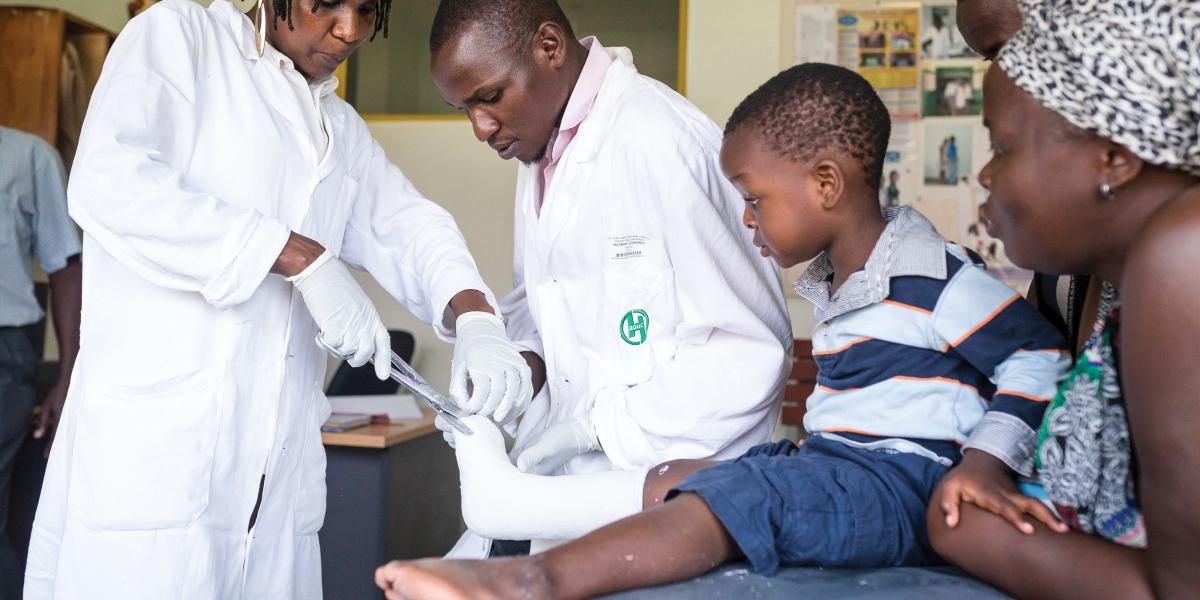
With Rehabilitation Care, ‘You Can Live Your Life Again’
By centering rehabilitation services in primary care, ReLAB-HS aims to expand access to this essential medical care.
The single mom in northern Uganda saved for three years to fund the 100-kilometer journey to repair her damaged prosthetic leg. During that time, she used someone’s discarded crutches as she struggled to tend her small garden. She injured her back in the process.
After she was fitted with a new prosthesis earlier this year, senior orthopedic technologist Azuruku Zackary of Gulu Regional Referral Hospital snapped several pictures of the woman outside a hostel where out-of-town patients can sleep. She is grinning, her black shorts revealing the smooth plastic prosthesis.
“She was really appreciative,” Zackary says. “She might go back to the garden and have something to put on the table for her and her children.”
In Uganda, these access challenges aren’t limited to people seeking artificial limbs. Zackary sees many people struggle to obtain rehabilitation care, from seniors with back pain to children with spina bifida who need wheelchairs or walkers. Rehabilitation services are concentrated in large urban centers, and travel is time-consuming and expensive. Too often, people forgo care entirely, at great cost to themselves and their families, he says.
A group of international partners led by the Johns Hopkins International Injury Research Unit (JH-IIRU) is working to improve access and availability through a five-year program called Learning, Acting, and Building for Rehabilitation in Health Systems, or ReLAB-HS. Launched in late 2020 and funded by USAID, the effort aims to bolster rehabilitation services in Uganda, Pakistan, Myanmar (Burma), and Ukraine.
Globally, 2.4 billion people—or 1 in 3—are currently living with a condition that would benefit from rehabilitation services, according to research from the WHO. Yet these needs are often unmet, especially in some low- and middle-income countries, where more than half of people can’t access necessary rehabilitation services.
Rehabilitation encompasses any health service that improves someone’s physical or cognitive functioning after experiencing an illness, injury, or disability. This can range from teaching someone with vision loss to use a white cane to supporting stroke survivors as they learn to move and talk again. Rehabilitation can lead to greater individual independence and break cycles that trap families in poverty, advocates say.
“With rehabilitation, everyone is allowed to reach their own potential,” says JH-IIRU director Abdulgafoor M. Bachani, PhD ’11, MHS ’08, an associate professor in International Health and director of ReLAB-HS.
JH-IIRU is working with several international partners whose expertise ranges from health systems to innovative rehabilitation service delivery. The initiative, which is funded through the Leahy War Victims Fund, selected Uganda, Pakistan, Myanmar, and Ukraine for their interest in improving health systems and integration.
“All of these countries have recognized this is a need and that rehabilitation needs will only increase,” Bachani says. “The appetite is big. The time is right. People are living longer, but with health consequences.”

Essential Services Close to Home
In many countries, people who live outside major urban centers are unable to access even basic rehabilitation services, such as strengthening exercises after a knee injury. ReLAB-HS is working to bring these services closer to people who need them.
The program is harnessing the power of community health workers (CHWs) to advocate for community needs and direct people to care. “They can be the eyes and ears on the ground, and identify folks who need rehabilitation,” says Nukhba Zia, PhD ’19, MPH ’13, an assistant scientist in International Health.
To that end, ReLAB-HS is piloting methods to help CHWs identify rehabilitation needs that people might otherwise dismiss, such as balance struggles. They’re also developing digital health tools CHWs can use for identification, referral, and management of rehabilitation needs.
CHWs can connect people to their local primary care clinics for diagnosis and care. Through a mix of online, hybrid, and in-person trainings, ReLAB-HS is teaching nurses and other primary care providers basic rehabilitation care, such as the correct way to use crutches or wheelchairs. For more complex care, they can make timely referrals to specialized rehabilitation centers. Even if someone must travel to a specialized center, the hope is to offer follow-up closer to home.
Technology will be a key component. ReLAB-HS is exploring the use of wearable devices to measure physical therapy progress. One partner introduced sensor technology that can document how long braces are worn to improve a clubfoot, for example, a congenital condition in which the foot turns inward and downward. The program is also addressing supply chains, looking at how to manufacture assistive devices in the countries themselves and how to create distribution hubs within the system.
Building and restructuring the way health care services and goods are delivered relies heavily on developing partnerships within a country, from the private sector to the government and professional organizations, says International Health assistant scientist Md Zabir Hasan, MBBS, PhD ’19, MPH, who works with ReLAB-HS.
Those collaborations have experienced some disruptions. For example, the war in Ukraine has largely stymied efforts there, while devastating floods and security challenges altered the program’s timeline in Pakistan. After the political upheaval in Myanmar, program leaders focused on private sector rehabilitation.
Another challenge arises in the need to quantify rehabilitation’s value to the broader society. ReLAB-HS is working to convince policymakers that rehabilitation is a worthy use of limited health funds. Despite its tremendous impact on an individual’s quality of life, rehabilitation is often not given the same priority as other pressing health needs like treating communicable diseases. Better data could demonstrate some of the far-reaching benefits.
In Uganda, ReLAB-HS is supporting the Ministry of Health to strengthen systems to collect data from health facilities on the number of people receiving assistive devices, rehabilitation services, and outpatient care, as well as improvement in individuals’ functioning. Having these figures will help quantify the need for services as well as highlight gaps, Hasan says.

Spreading Awareness, Reducing Stigma
Behind those numbers are untold stories of people whose lives are changed, says Sarah Magoba, who supports ReLAB-HS communications in Uganda. Magoba often thinks of a mother who has a child with cerebral palsy. When the child was born, the woman’s husband left her.
“People think it’s a curse to have a disabled child,” she says. “With that stigma, so many mothers hide their child.”
This mother carried the preschool-age child on her back about 8 kilometers to work, where the nonverbal child would lie flat all day in the daycare. Access to a wheelchair improved both of their lives.
“The mother started seeing hope in the child that the child could get better,” she says. “The load was lighter.”
Magoba says she’s hopeful the ReLAB-HS effort will spread the knowledge of rehabilitation’s potential to more people, reducing stigma in the process. CHWs will be key to this effort.
“People trust them and believe in them,” she says. “They’re the first line of information.”
In Pakistan, ReLAB-HS is taking a similar community-based approach, working with Lady Health Workers, a group that has made significant strides in improving health indicators there.
Disseminating information and education about rehabilitation on a community level could help more people reap its tremendous benefits, says advocate Ghulam Nabi Nizamani, who uses a manual wheelchair after contracting polio.
“Still now many people are confused about what is the rehabilitation and how it can work side by side with the health professionals,” he says.
Nizamani envisions a better future for the young people he’s seen with spinal cord injuries who are bedridden at home. He wants to see these individuals supported in an upright position, managing their daily life through well-fitted assistive devices such as braces, wheelchairs, and walkers.
“They could live a life independently,” he says.
In Uganda, Alex Munyambabazi has seen firsthand how access to rehabilitation services can benefit the individual and society. He lost a leg after stepping on a land mine when he served in the military nearly two decades ago.
After struggling with stigma and loss, he started moving around the capital in his shorts, proudly displaying his prosthetic limb. He mentored others with amputations and formed a foundation called Amputee Self-Help Network Uganda. Now, the father of two is in his fourth year of medical school. He wants to help people with all aspects of rehabilitation, from amputation to physical therapy and counseling.
“Losing a limb is just an obstacle,” he says. “You can live your life again.”